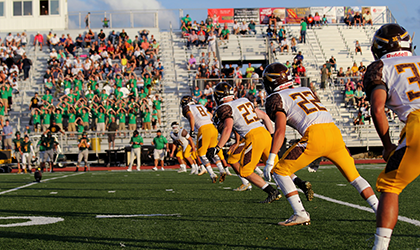
Universities around the United States are struggling to deliver their “product” in a manner that preserves its educational and social value. By design, universities draw people together as part of the learning process. Covid-19 challenges this objective, requiring students to distance themselves and not gather in large groups. This conflict is forcing universities to rethink their business models, transforming what they do in a manner that adds value while protecting everyone’s health.
Intercollegiate sports, for example, are a significant component of student activities at many universities in the United States, yet Covid-19 resulted in the cancellation of all winter sports championships and spring sports in March 2020. This decision was consistent with numerous states closing their economies to protect their residents from a new coronavirus of which little was known.
Since that time, much has been learned about Covid-19, including who is most vulnerable and what steps can be taken to suppress the spread of the virus. In general, the older a person is, the more likely that they experience a poor outcome if infected. People with underlying health conditions, like diabetes and obesity, also experience similarly poor outcomes at a higher rate than those not so afflicted.
Data have become available since March 2020 to inform the risks associated with Covid-19 infections. Risk mitigation informs decision-making in the presence of risk. The subjective component is how much risk is acceptable or tolerable, and what steps can be taken to limit its impact. For example, if one never wants to be in an airplane crash, the solution is to never fly. This creates unintended consequences, such as if you only drive in an automobile, the accumulated risk of automobile travel accidents and fatalities quickly exceeds the risk of flying.
The same principle applies to college team sports. To quantify the population risk of playing such sports, one must ask what the risk is of playing, and the risk of not playing. First the risk associated with just being an 18-24 year-old in society can be quantified based on historical data.
Consider the 130 college (American) football teams that are part of the Football Bowl Series (FBS). We assume that each of these teams have 100 players on average, giving 13,000 players overall. We also assume that the football season covers six months, including summer workouts prior to the beginning of the season.
Looking at United States’ Centers for Disease Control and Prevention (CDC) data reported from 1 March 2020 through 30 May 2020, there were approximately 75,000 confirmed cases among 18-24 year-old men, resulting in approximately 450,000 infections in this group (using a 6 to 1 ratio between infections and confirmed cases estimated by the CDC). Given that there are just over 15 million people in the population in this age group, this works out at a 3% infection rate.
The CDC also estimated that there were 67 Covid-19 deaths in the male 18-24 age group during this time period. Using all this data, the first row in Table 1 gives 99.9% one-way confidence interval upper bounds for the expected number of deaths amongst all 13,000 college football players as a function of their infection rate. This upper bound provides a worst-case scenario for expected number of player fatalities. Table 2 gives 95% confidence intervals for the same statistics.
University athletic departments have kept infection rates down by employing team bubbles, which limit player exposure to infection risk by creating a set of protocols that players follow not only while playing and practicing, but during classes and down time. Player buy-in has created an environment that maximizes player safety, designed to keep infection rates amongst the student athletes lower than the general student population. This means that the expected infection rate amongst FBS players may remain below 10%, resulting in an environment where the risk of even one death is unlikely.
To place these numbers in perspective, over the past 10 seasons (2010 through 2019) there have been 42 FBS player deaths, including both non-football related accidents and shootings, and football-related health deaths. In addition, from 1 March 2020 through 30 May 2020, for 18-24 year-old males, the CDC reported 4,337 non-Covid-19 deaths. Scaling this over a 13,000-person cohort over this three-month time period gives 3.7 deaths. What this suggests is that if college football is played, the Covid-19 fatality risk is negligible, provided the infection rate can be kept low.
The same data analysis can be done for Division I men’s and women’s college basketball, women’s volleyball and soccer, and men’s and women’s golf. The 99.9% one-way confidence interval upper bounds and 95% confidence intervals for the expected number of student-athlete deaths for each of these sports is a function of the total number of student-athletes participating, the gender, and the length of the season (including preseason training and postseason play). All these values are reported in Tables 1 and 2.
Table 1: Expected number of student-athlete deaths (99% one-way confidence interval upper bounds) at different Covid-19 infection rates.
| Sport | Number of athletes (estimated) | Length of season (months) | Infection rate | |||
| 5% | 10% | 15% | 20% | |||
| Football | 13,000 | 6 | 0.36 | 0.71 | 1.07 | 1.42 |
| Men’s basketball | 5,557 | 9 | 0.19 | 0.38 | 0.58 | 0.77 |
| Women’s basketball | 5,085 | 9 | 0.11 | 0.21 | 0.32 | 0.42 |
| Women’s volleyball | 5,582 | 6 | 0.08 | 0.15 | 0.23 | 0.31 |
| Women’s soccer | 9,588 | 6 | 0.13 | 0.27 | 0.40 | 0.53 |
| Men’s golf | 2,941 | 10 | 0.13 | 0.27 | 0.40 | 0.54 |
| Women’s golf | 2,220 | 10 | 0.05 | 0.10 | 0.15 | 0.20 |
Table 2: Expected number of student-athlete deaths (95% confidence intervals) at different Covid-19 infection rates.
| Sport | Infection rate | |||
| 5% | 10% | 15% | 20% | |
| Football | (0.10, 0.28) | (0.20, 0.56) | (0.29, 0.84) | (0.39, 1.13) |
| Men’s basketball | (0.06, 0.18) | (0.13, 0.36) | (0.19, 0.54) | (0.25, 0.72) |
| Women’s basketball | (0.03, 0.09) | (0.07, 0.17) | (0.10, 0.26) | (0.14, 0.34) |
| Women’s volleyball | (0.03, 0.06) | (0.05, 0.12) | (0.07, 0.19) | (0.10, 0.25) |
| Women’s soccer | (0.04, 0.11) | (0.09, 0.21) | (0.13, 0.32) | (0.17, 0.43) |
| Men’s golf | (0.04, 0.11) | (0.07, 0.21) | (0.11, 0.32) | (0.15, 0.42) |
| Women’s golf | (0.02, 0.04) | (0.03, 0.08) | (0.05, 0.12) | (0.07, 0.17) |
These results suggest that with the appropriate precautions in place to keep infection rates low, numerous team sports can be played with minimal fatality risk to the student-athletes.
In August 2020, the Big 10 and the Pac 12 athletic conferences – involving universities from the midwest and northeast, and western United States, respectively – cancelled all fall sport competition, with college football the most visible sport affected. The factor that appeared to contribute to this decision was the risk of myocarditis, an inflammation of the heart muscle typically caused by virus infections. The unknowns associated with this condition created additional risks that may have prompted the cancellation decision.
There is limited data available to assess this additional risk. What is known is that if a student athlete does not get infected, then the risk of myocarditis due to Covid-19 is zero. Therefore, the best way to eliminate this risk is to keep students athletes from becoming infected. For those students who have been infected, the best strategy to reduce myocarditis fatality risk is to medically screen such people to identify any cardiac abnormalities. If one wanted to be even more risk averse, all student athletes who have tested positive in the past can be banned from participating in their sport this season. For college football teams with 100 players, this could mean that as many as 10 student-athletes would not be permitted, though it is likely to be much lower. Note that in mid-September, both athletic conferences reversed course and opted to play football, and schedule other fall sports. With this about face, they instituted significant medical screening protocols, including daily infection testing, setting a high bar for player safety and well-being.
Managing and mitigating risk is the best approach to take for planning how to hold college team sports competitions. Running away from risk often creates additional unforeseen problems. Lessons learned from professional sports like baseball, hockey, and basketball suggest that team bubbles are effective to keep players infection free over extended time periods. The same principles can be applied to college team sports, opening a pathway for them to be held, even with the threat of Covid-19.
About the author
Sheldon H. Jacobson is a founder professor of Computer Science, director of the Simulation and Optimization Laboratory, and founding director of the Bed Time Research Institute at the University of Illinois at Urbana-Champaign.